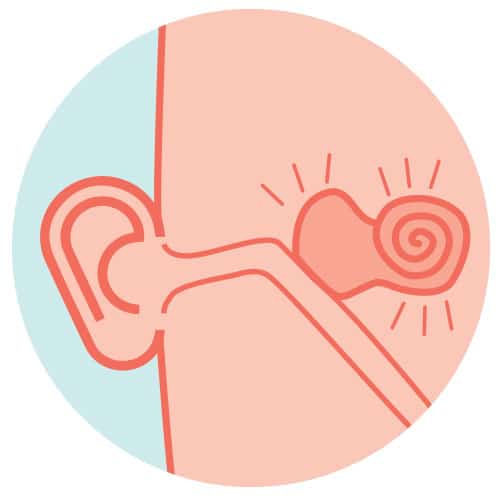
The outer ear (pinna) is designed by nature to work like an acoustic antenna. It helps the brain localize and tune in to a particular sound, for example when listening to a specific voice in a crowded café. However, the most popular styles of hearing aids (Receiver-In-Earand Behind-The-Ear models) capture sound from microphones that sit behind the ear and then approximate the effect of the pinna. The result is an averaged and incomplete reproduction of sound, making it hard for the brain to achieve its natural localization and noise-cancelling function. In fact, of the 79 million people who wear hearing aids globally,1 93% report having trouble hearing in noisy environments and 55% get confused about where sounds come from.2
ReSound ONE is the world’s first full-featured* hearing aid with a Microphone & Receiver-In-Ear design (M&RIE) that uses the unique shape of every individual’s ear to collect sound. This remarkable innovation has been achieved with a radical new receiver system combined with all-new Digital Feedback Suppression (DFS Ultra III) enabled by GN’s new and most powerful sound-processing chipset ever. By picking up sound directly inside the ear, ReSound ONE gives the brain everything it needs to tune in to individual voices, as well as significantly reducing background noise. Clinical studies show that all hearing aid users benefit from listening to sounds collected with their own ears, with 90% of users preferring the sound quality of ReSound ONE with M&RIE instead of only the microphone behind the ear.3&4
GN Hearing CEO and President, Gitte Aabo explains, “I am very proud that, once again, GN is first in the industry with ground-breaking innovation that will make a genuine difference in how people experience conversations and sounds around them. Placing a microphone into the ear with an open-fit hearing aid is something the industry has battled for many years to achieve. This technology will allow people with hearing loss to feel that they are literally getting their own hearing back and hearing the way nature intended. ReSound ONE will boost the communication, relationships and confidence of every individual.”
Additionally, ReSound ONE incorporates new All Access Directionality and the user-activated Ultra Focus settings. These enhanced operating modes significantly improve speech recognition while preserving spatial perception in complex sound and noise situations. ReSound ONE includes unmatched rechargeability and extensive connectivity options to both iOS and Android™ smartphones for streaming and hearing aid control.
ReSound ONE is available from August 27, 2020 in rechargeable and non-rechargeable models. This technology is also available in new Beltone Imagine hearing aids.
For further information, visit the ReSound Newsroom and read more about the Organic Hearing philosophy.
Learn more about GN’s 2020 and beyond strategy with focus on individualized customer experiences.